Trabeculectomy
Trabeculectomy is an operation used in the treatment of glaucoma and it involves the creation of a fistula between the inside of the eye and the space under the conjunctiva, the clear tissue covering the white of the eye. It allows fluid to drain out from the inside of the eye into this space, thus lowering the pressure in the eye. The surgery can be performed under local or general anaesthetic and takes around an hour to perform.
The conjunctiva is peeled back, a bit like the cuticle on a fingernail, and a rectangular flap is made in the stiff white part of the eyeball (the sclera). An opening is made under the flap into the eye, removing a section of sclera and a section of the iris, to stop it from plugging the opening.
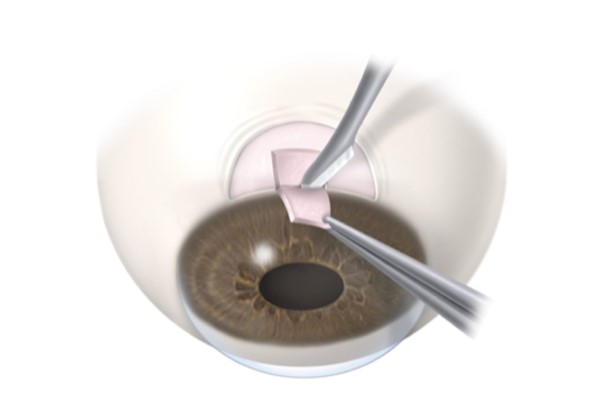
The scleral flap is then stitched back using a fine section of suture made of nylon. The stitches are adjustable/removable so the flow of fluid from inside the eye can be controlled. The conjunctiva is then repositioned over the sclera and stitched back down into place.
The site of surgery is usually under the upper lid so is not visible directly but a blister or ‘bleb’ can be seen if the upper lid is lifted. This is the site to which the fluid drains from inside the eye and from there it diffuses away into the vessels over and around the surface of the eye.
Frequent follow up is required, usually on day 1, and then weekly for a number of weeks and the aftercare is as important as the surgery itself. As with any cuts made in the body, scarring can occur and this drainage channel can shut down. There are a number of ways, this scarring is minimised. First, during the surgery, an anti-scarring drug is used (either Mitomycin C or 5-Fluoroural) and after the operation, steroid drops are prescribed, along with antibiotics. The steroid drops are usually prescribed 2-hourly for a minimum period of 2 months.
If the flow slows, the stitches can be released to open the flap and increase the flow. Often, a small procedure called a needling is used to break up the scar tissue and a small amount of anti-scarring drug is added to help keep the flow out of the eye going and to keep the bleb functioning. This can sometimes be done in clinic but often is done in the operating theatre.
Trabeculectomy aftercare is complex and there are a number of potential problems or complications after surgery:
- The stitches can be irritating – these are often removed and will not cause a problem past the first few weeks
- At the initial visit, there is a chance the pressure can be too low, which may be due to a leak or an over-draining bleb. Further procedures may be required in either situation such as refilling the eye with viscoelastic to keep it formed or re-suturing of the eye.
- If the pressure is low after surgery, the inner layers of the eye can collapse inwards (choroidal effusion) and cause shadows in vision. These usually settle after the pressure returns to a more normal level. Occasionally there can be bleeding into the eye and this can lead to sight loss but this is rare.
- There is a change in the glasses prescription after trabeculectomy surgery – as the shape of the eye changes afterwards slightly (astigmatism).
- There is a risk of infection getting in – this requires a large incision so there is a higher initial risk and also an ongoing yearly risk of getting infection in the eye as the wall of the bleb is thin and bacteria can cross this to get into the eye. During surgery, we take great care to clean the surface of the eye with iodine but bacteria get into the eye in 1 out of every 1000 operations and this can lead to sight loss. You will be advised of symptoms to look for but they include a sudden increase in pain, redness or drop in vision in the few weeks following surgery.
- There is acceleration in cataract formation/development after trabeculectomy surgery
If both cataract surgery and trabeculectomy surgery are needed, they can be performed at the same time, although this has a slightly lower chance of success than performing the trabeculectomy surgery at a separate time. If cataract surgery is performed, then it is usually best to perform the trabeculectomy surgery after a few months to minimise inflammation from the cataract surgery. If the trabeculectomy is performed first, it may fail or become less effective if a cataract operation is subsequently performed due to the inflammation that arises after cataract surgery. Performing both together is however more convenient and may be necessary if the glaucoma is progressing and cataract surgery is simultaneously required.