Eyelid Lesions
Eyelid Papilloma
Papilloma of the eyelid are benign tumours and carry little to no risk of change to any form of cancer. They can be solitary or multiple and can either have a smooth or rough (corrugated) edge surface and they are usually of a similar colour to the surrounding skin. They may cause mild irritation or may be cosmetically unacceptable to the patient. There are a few different sub types of papilloma and the most common is the squamous papilloma, otherwise known as a skin tag. This is usually soft flesh coloured smooth or pedunculated. Seborrhoeic keratosis is another benign proliferation of cells which has a ‘stuck on’ appearance and can be variably pigmentated. Their colour can vary from pink or flesh coloured to dark brown. They are usually well circumscribed and elevated often with an inflamed base (the Leser Trelat sign). The appearance of multiple separate keratoses in one area can suggest a para neoplastic process. Inverted follicular keratosis is usually a solitary lesion of the eyelid margin, which may or may not be pigmented and can be of a nodular papillary in appearance and finally the verruca vulgaris is a flesh-coloured growth caused by the human papilloma virus and this can also be found on the eyelid.
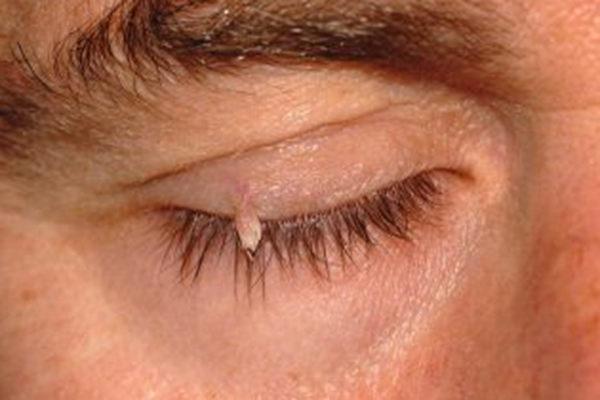
These lesions can be observed however if causing irritation or if cosmetically unacceptable they can be removed. Removal usually involves local or shave excision under local anaesthetic however verruca vulgaris often responds better to cryotherapy. Larger eyelid papillomas may require intralesional interferon therapy. If there is any suspicious characteristics, then the lesion may be sent to pathology to exclude any sinister differential diagnosis.
Chalazion and Styes
A stye is a small red painful lump that grown at the base of your eyelash and these are often caused by a bacterial infection. The eyelid is often red and tender to touch, and the eye may feel sore and scratchy. Eyelid inflammation or blepharitis can result in a predisposition to getting styes and it is worth treating these conditions to prevent recurrence.
Chalazion is a blocked oil gland or meibomian gland and may start as a stye or internal hordeolum. These tend not to be red and painful to start with and often appear as a pea size lump in the body of the eyelid. If they become large, they can press on the eye and cause your vision to become blurry.
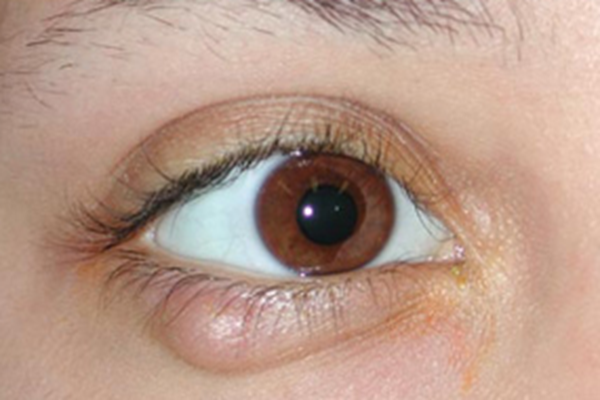
Often both styes and chalazions can settle on their own and hot compresses are helpful as they help express the material from the glands. The heat melts away any blockage at the entrance of these glands. Hot compresses are best done by holding a clean flannel under hot water pressed firmly against the closed eye for 5 to 10 minutes, ideally 3-4 times a day. The warm compress helps to soften the contents of fluid filled swelling and the pressure helps express the contents. Antibiotic ointments are not usually of benefit for a chalazion. However, if there is an acute red tender area as in a stye, then a course of antibiotic ointment may of some benefit. Ongoing cleaning of the eyelid with a weak solution of baby shampoo and warm water or over the counter eyelid wipes such as Blephaclean or Optase helps to remove grease and dead skin cells that can predispose to cyst formation.
If the above conservative treatment has not helped, then a small operation can help to drain the contents of the cyst. This is usually done under local anaesthetic but can be done under general anaesthetic in children or in adults that may not tolerate this. A small cut is made on the inside of the eyelid and the contents of the cyst are removed with a curette. Antibiotic ointment is usually prescribed afterwards, and the results are normally excellent.
There is a chance for recurrence and hot compresses are helpful on an ongoing basis to reduce the change of recurrence.

